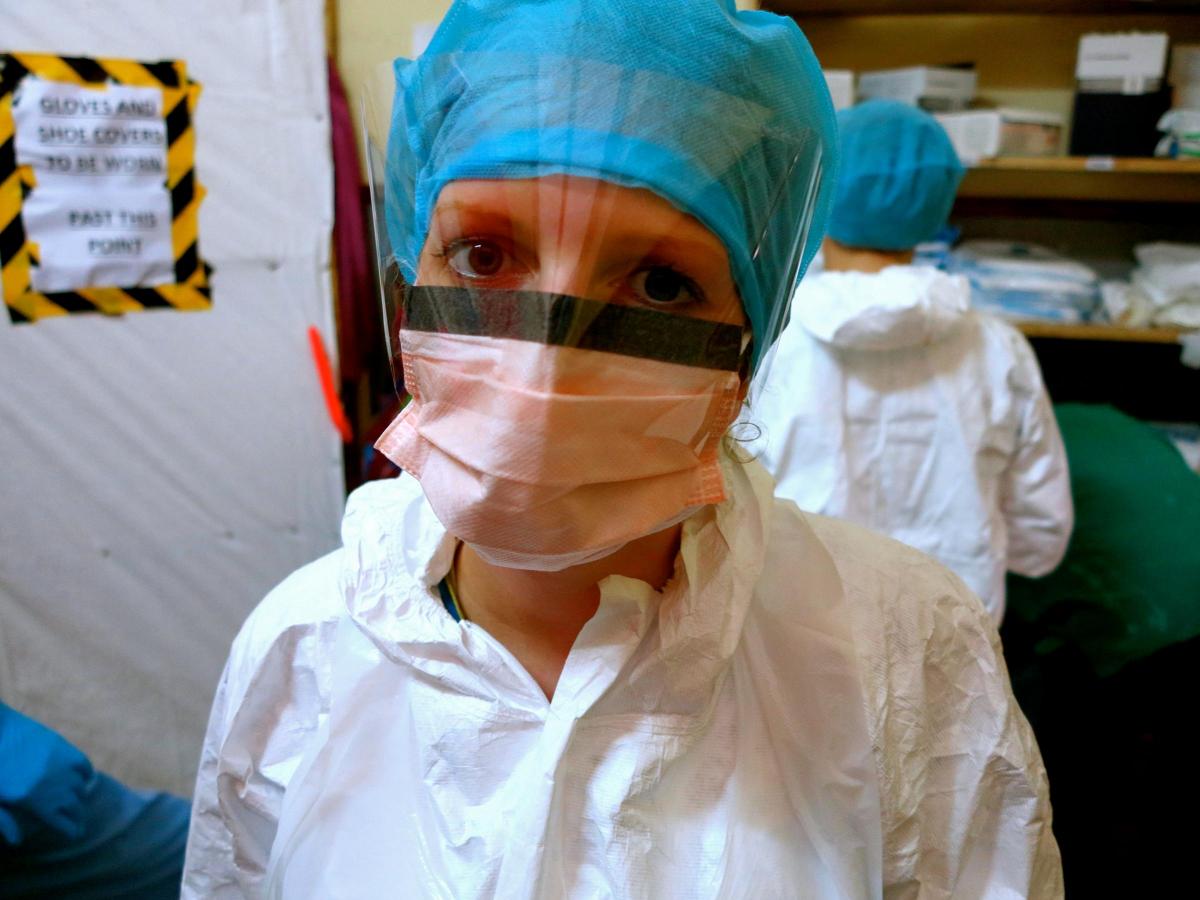
SHE may be smiling for the camera but brave Basingstoke nurse Natalie Mounter is actually working in a heartbreaking and hellish environment.
32-year-old Natalie decided to quit her job as an isolation ward nurse at Basingstoke hospital to help people affected by the devastating Ebola outbreak in West Africa.
Natalie is now part of a UK medical team that is bringing vital aid to the victims of the worst outbreak of the deadly disease since the virulent virus was discovered nearly 40 years ago.
This week, Natalie sent The Gazette an exclusive despatch from the frontline of the fight to help Ebola victims in Sierra Leone:
"This is my first experience of working in Africa, and my first trip to Sierra Leone.
Freetown is a vibrant city but it is poor – the health system is lacking in so many resources and the conditions in which many people live can be heartbreaking.
It is easy to see how this country was not prepared for a disease like Ebola, which was previously unknown and so deadly.
Things here are unpredictable and often chaotic. We are working in an emergency situation and so new challenges are constantly arising and we have to try to adapt and respond to things as they happen.
Like all other clinicians here, I work six-hour shifts on the isolation unit six days a week. I spend up to three hours a day in personal protective equipment (PPE) on the ward. What I do during and outside of these shifts can vary enormously, depending on what arises.
I work with a team that includes several Sierra Leonean nurses, who are fantastic. This is one of the most enjoyable parts of my role. Doctors, nurses and cleaners all work together to achieve the same goals, teamwork is extre-mely important when working in such a dangerous job.
When we’re inside the unit, dressed in PPE, we give basic medications, clean and change patients that have had diarrhoea and vomited, feed people who are too weak or confused to do it themselves and try to give as much comfort as we can.
Even though we work hard to give care to our patients, it often feels that with limited treatment and no current cure available, we can’t do much to relieve their suffering. This can often be difficult to deal with on an emotional level – to watch people suffer and feel almost helpless to do anything.
Recently, we have had a number of children on the ward. This is undoubtedly an extremely distressing and frightening situation for them. They don’t understand what is happening, they are without their parents and are often very unwell.
It can be hard to provide them comfort as we are always dressed in PPE and many of us don’t speak the local language yet. The suffering of children is the most distressing element of my job, and it is something that everyone here finds difficult to deal with.
When I’m not on the ward, I’m trying to work with, and train, local nurses in infection control and look at ways in which we can reduce risk to the health care staff and our patients. The nurses are very receptive and keen to learn.
I also visit other centres that King’s is involved with and meet people from other agencies who are out here to work out ways to improve treatment centres and make them safer for staff and patients."




Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules here