SHE just wanted to have a blemish removed from her forehead – but a Basingstoke mum endured an agonising ordeal and has been left with blurred vision in one eye after suffering a bad reaction when a drug used for varicose veins was injected into her face.
Lisa Fairbanks went to her doctor after a blood dot appeared on her forehead, but was advised that treatment was not available on the NHS, and it was suggested she try a beauty clinic.
The mother-of-two, from Cran-bourne, researched various clinics and found one based in St John’s Piece, Oakley, called pureSkin.
Lisa said: “I came across Julie Kenny. She has a very professional website and she’s a member of the Nursing and Midwifery Council. She looked at the blood dot and said ‘no problem’, and told me that she would inject it. She said it would flush it out.”
Ms Fairbanks agreed to go ahead with the treatment last October, at a cost of £55, and said a substance called Sclerovein was injected into the dot three times. However, it was quickly clear something was wrong.
The 40-year-old said: “It was shockingly agonising. I said: ‘I can’t bear the pain any more’. She attempted to do it again, and said she wasn’t happy, and said that she wouldn’t charge me. She said hopefully it would go away.”
But as Lisa was driving home, her face started to swell. The next morning, she woke up with further swelling, a feeling of immense pressure behind her eyes, and blurred vision.
She contacted the Evolutions Clinic, in Winchester, for advice, and Andy Tait, co-owner of the company, told her to go to the hospital emergency department.
Lisa visited the emergency department at Basingstoke hospital where she said she was told that Sclerovein was the cause of the problem in her case, although the drug is normally quite safe to use on varicose veins.
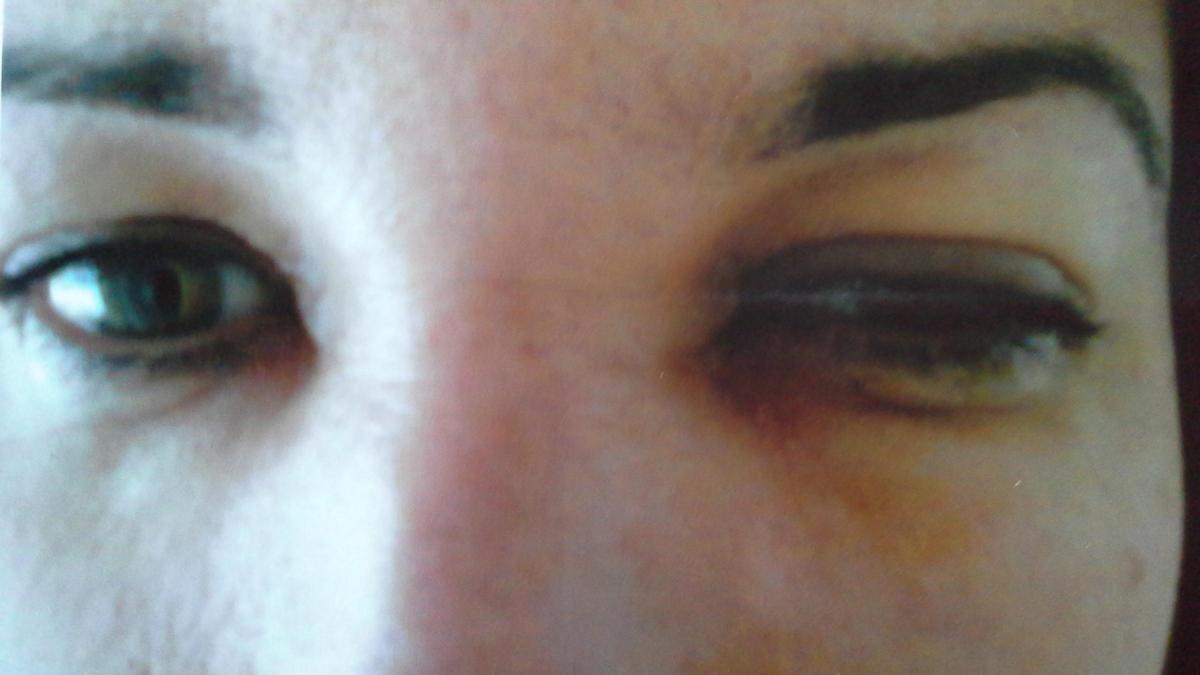
She said: “My face looked like it had been in a boxing ring. I couldn’t see out of my left eye at all. My vision had gone.”

Lisa, who works in a beauty salon, said she has been left with pain behind her left eye, headaches, blurred vision and a scar on her forehead.
Lisa has since had to pay £940 for further remedial treatment, and said the ordeal has knocked her confidence.
She added: “I feel really depressed. I have changed my hairstyle and I talk about it all the time. I’m not stupid – I did my homework.”
Mr Tait, who specialises in treating skin blemishes, told The Gazette that he has never heard of sclerotherapy treatment being used on the face.
He said that had Lisa attended his clinic, he would not have injected anything in her face to treat the blood dot, adding: “I use the hot tip of a blunt needle to shut the vessels down.”
Although sclerotherapy is not prohibited from being used on the face, it does carry certain risks. A similar case was reported in the media earlier this year, after a nurse performed sclerotherapy on a patient in May 2010, which resulted in the patient’s face swelling.
The Nursing and Midwifery Council heard that the patient was left with a small indentation on her cheek.
The nurse involved was cautioned after the NMC panel said: “Although this treatment can be used for veins on the face, it should not be done without fully informing the patient of the risks involved, obtaining an appropriate prescription, and obtaining the patient’s informed consent.”
Lisa contacted the NMC to report what had happened. In May this year, the council placed various interim conditions on Julie Kenny for 18 months whilst it carries out an investigation.
These include that she has to produce a personal development log detailing the consultation process and risk assessments undertaken before she provides “any invasive cosmetic treatment or procedure”.
A copy of this log must be forwarded to the NMC within 28 days of the date on which the conditions become effective.
Ms Fairbanks took her complaint to solicitors Penningtons Manches. But even if she had a legal claim, she was told she would be unlikely to receive any compensation because Julie Kenny was not insured for the treatment she administered.
Elise Bevan, senior associate in the clinical negligence team at the solicitors, said: “This is a classic example of unregulated treatments being performed. While the treatment may seem straightforward and simple, the consequences when it goes wrong can often be catastrophic.”
She explained that at the time, it was legal for aesthetic practice to be excluded from insurance, but this was changed in July by the Royal College of Nursing.
When contacted by The Gazette, Julie Kenny declined to comment.
The British College of Aesthetic Medicine states on its website that sclerotherapy treatment was developed in the 1920s for the treatment of varicose veins.
Complications that can arise from its use include allergic reactions.




Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules hereComments are closed on this article